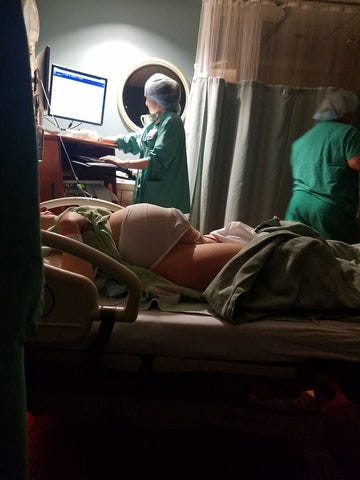
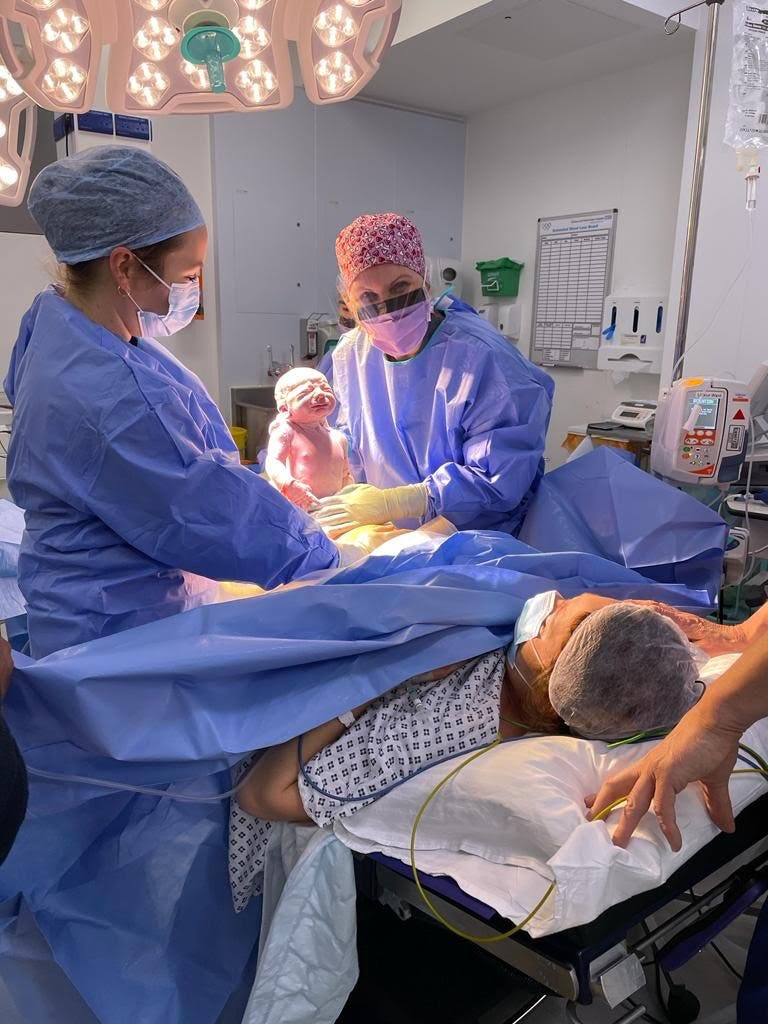
Joys & Scars: The Realities of Cesarean Birth
A surgeon, pelvic floor therapist and mother share their expertise.
Throughout the process of putting together this edition of Body of Knowledge, I was uplifted by the number of positive stories surrounding cesarean birth. From London-based Obstetrician Dr. Gergana Peeva who spoke so joyfully about the “Lion King” moment of a cesarean delivery to Nyssa co-founder, Aubrey’s declaration that “there is so much magic waiting for you on the other side,” I came away from these interviews with an even greater sense of awe and respect for those who deliver via c-section. Cesarean section rates are on the rise worldwide– currently over 1/3 of all births in the U.S. are c-section deliveries . But despite the prevalence of the procedure, misconceptions and ‘unmentionables’ abound. Like so many topics we discuss on Body of Knowledge and with Nyssa, we wanted to take this opportunity to help break the stigma and set the record straight.
Did you give birth via cesarean? Are you planning to? Or know someone who is? We would love to keep the conversation going in the comments. What resonated with you? Do you have any questions for our professionals? Experiences to share with other readers? Comment below to be in to win a copy of Dr. Pooja Lakshmin’s amazing new book, Real Self Care (she gave birth via c-section, too!).
Warmly,
Mia x (Editor-in-Chief, Body of Knowledge)
A Mother’s Joys & Scars: Co-Founder of Nyssa, Aubrey Howard, Shares About Her Unplanned Cesarean Birth
Nyssa co-founder, Aubrey, lives in Michigan with her 6-year-old son. She shares her experience of navigating an unplanned c-section and the emotions that arose afterwards.
“I’m pretty sure that hospital maternity departments schedule progressively better nurses the closer patients are to the ‘zero hour’ of birth. In theory, that’s amazing. I certainly want the best medical team overseeing that life-changing moment. In practice, this meant the nurse with poor bedside manner and the touch of an iron fist in a sandpaper glove was tasked with pushing a cervix-softening pill deep into my vaginal canal, kicking off what would be my three-day birthing extravaganza.
The pregnancy that led to the existence of my beautiful six-year-old boy was very wanted, albeit very unplanned. That modern augur – the fine lines on urine-soaked plastic – marked the eminent change and magnitude of unknowns. Planned or unplanned, finding out you’ll have your first child dramatically changes how you observe the world around you, and the countdown begins.
Now, when I scrolled through my Instagram feed, it was with novel attentiveness toward former high-school chums, smiling through tears and exhaustion, triumphantly snuggling the little bundles that they had just heroically pushed out of their bodies.
I quickly absorbed terms like ‘empowered birthing,’ ‘breast is best’ and ‘vbac.’ I watched an inordinate number of videos in which women, held from behind by their shirtless partner, squatted in a pool of water as a dark form appeared and surfaced… poof! A baby! The mother crying and laughing from sheer overwhelm.
As the countdown continues, the reality of what’s ahead sharpens focus. And, like every human I’ve ever met preparing to give birth for the first time, the countdown also made me scared. Scared of pain, scared of uncertainty, scared for the health of this new love living inside me.
It’s fascinating how when we are feeling scared, there seems to be a compulsive, collective societal response to make us un-scared. Choruses of ‘your body was built for this – it will know what to do’ or ‘women have been doing this for Millenia’ began to infiltrate many of my conversations. (In case you don’t finish this: Never ever say any of these things to a pregnant person).
I sped through my pregnancy with mounting rapidity and cognitive dissonance. Yes, I’m about a foot shorter than my partner and he was over 9 lbs at birth…but I will access this magical experience of empowered birth. Sure, most women in my family have given birth via emergency cesarean…but I don't want any medical interventions. After all, it all really seems to be a matter of willpower. Of preparation. Of strength. Right?
My due date – the first due date, at least – was Thanksgiving of 2016. I was terrified and excited as it came and went.
At my next Doctor’s visit, they concluded that the first due date had been wrong. They pushed it back a week. I walked a lot, tried to get my partner to have sex with me (not to connect or enjoy, but because the doctor had advised that the best way to get a baby out is the same way it got in).
Due date pushed back one more week.
Having lost all motivation, I spent the week on my couch with my friend, Cognitive Dissonance, watching Frasier and eating *a lot* of frozen custard.
Scheduled for induction.
A few days before my ‘appointment,’ exhausted, uncomfortable, I now woke up with unbearable itchiness. Using my phone to photograph the underside of my belly (now a blurry artifact of the stretchmarks I had so proudly avoided) and found red lines expanding. Like pulling the loose thread on a woven sweater. I was unraveling.
The induction date arrived. On the elevator, hilariously stressed about being late for what would actually be a week and a half stay in the maternity ward, I kept thinking about what my mom said about her c-section with me: ‘You had the most beautiful, perfectly round head.’
I looked in the stainless-steel reflection. When and how did my belly get this big? My mind flashed back to and fixated on one of my birthing classes where we covered the ‘cascade of interventions.’ When you say yes to one, more inevitably follow. My first intervention was the vaginal pill. The one delivered by Nurse Sandpaper. The reason I’m here, on this elevator, right now.
I could talk forever about the process of my own emergency c-section. The back labor (which I hear happens more often when induced), how, lying on the operating table I couldn’t stop thinking about the fact that I’d had the same anesthesiologist for the last 36 hours (and was he falling asleep in his chair?), not being able to move or breathe while they pulled out my son…
I could also talk about way that women are poorly served by the modern healthcare industry, how messed up it is that pregnancy is considered a pre-existing condition for insurance, the history of disempowerment of women to advocate for their own health, the breathtakingly abysmal treatment of women of color resulting in one of the most atrocious maternal mortality rates in the modern world…
All these things are so, incredibly important.
I was lucky/privileged enough to come out on the other side of my emergency c-section with a healthy baby, no complications, and well cared for by a team of kind and competent medical professionals (yes, I’ll even include Nurse Sandpaper in that count). But I also came out on the other side with a deep sadness. Did I miss out on an opportunity to connect with the primal forces of nature? To experience spiritual and physical transformation? Should I have done more prenatal yoga? Prepared differently?
As it is wont to do, time passed. I learned to say, ‘vaginal birth,’ instead of ‘natural birth.’ Those worries became consumed by new, different worries. ‘Is it normal for my son to stick his finger up his butt?’ and ‘how the hell do modern families afford childcare?’ Etcetera.
But recently, a good friend’s sister had her first child. I asked how the sister was faring with her postpartum recovery, and my friend shared how saddened, how disappointed, her sister was. She’d wanted to give birth ‘naturally,’ and had to have her own emergency c-section.
Yes, the sister had big plans for the magic of birth. And there’s absolutely nothing wrong with that sadness, or for wanting to avoid medical intervention, or for disappointment when important events don’t unfold according to plan.
But there is a problem with the narrative of the ideal birth. With the guilt. With the notion that despite the pressure put on modern families to stay afloat, despite the chronic disempowerment of women in healthcare settings, despite all of this: women and birthing folks feel personal responsibility to ‘live up’ to what ‘their bodies are built for.’
This narrative doesn’t prioritize the health of parent and child. It doesn’t account for societal and political responsibility to care for those birthing and raising the next generation of humans. And it doesn’t equip us with the information that we need to not only make the best decisions for ourselves, but to experience less trauma (I, for one, didn’t go to the gynecologist for two years after the birth of my son. Thanks, Nurse Sandpaper).
So, if you know someone who is about to give birth, listen to them, encourage them to learn more about advocacy in a medical setting, and do not tell them that people have been doing this for millennia. Because people have also been dying doing this for millennia.
And if you’re about to give birth: I may not have connected with the elusive ancient mysticism, but I can tell you from experience that there is so much magic waiting for you on the other side. And if you do end up having a planned or unplanned cesarean, yes, it is a major surgery (and I, for one, look like death warmed-over in all photos). But I’m alive. My baby is alive. And my vagina is in pretty great shape. (No thanks to Nurse Sandpaper).
Original article.
An Obstetrician’s Perspective on Cesarean Birth: Advice from Dr. Gergana Peeva
Nyssa Network member, Dr. Gergana Peeva, is a consultant in Obstetrics, Gynecology and Fetal Medicine based in London, U.K. Through her private practice (and many years with the NHS), she is dedicated to empowering and supporting women throughout their pregnancy journey as well as providing comprehensive fetal medicine expertise. In this video interview, Dr. Peeva shares her perspective on preparing for a c-section delivery, recovery after birth, handling common myths and misconceptions and much more.
Physical Therapy Following Birth: An Interview with Physical Therapist and Pelvic Health Specialist, Dr. Celestine Compton
“No one is expected to "figure it out" or "deal with recovery" on their own following an injury or a surgery. Why should birthing a baby be any different?" Nyssa Network member, Dr. Celestine Compton, is a doctor of physical therapy who specializes in women’s and pelvic health. She also works with our friends at Origin, which offers virtual and in-person visits for pregnancy, postpartum, sexual health, and menopause. I reached out to Celestine to discuss pelvic health for women after vaginal and cesarean birth.
MC: Please can you explain the ways in which physical therapy can play a role in helping people heal after birth and if/how your practice differs depending on whether you’re treating someone who has had a vaginal or c-section delivery?
CC: After delivery, most people are not given adequate guidance about how to care for their postpartum body, what signs and symptoms to be on the lookout for, and how to best promote healing, whether following a vaginal or cesarean birth. Physical therapy aims to fill that gap in postpartum health care.
When working with a physical therapist, whether days, weeks, or months postpartum, they are concerned about what your current function is, what tasks or activities may be painful, difficult, or impossible for you to perform, and what specific goals you have following delivery. Your physical therapist will take all of this into consideration, along with your pregnancy and birth experience, in order to develop a plan of care that is specific to your needs. Treatment is individualized and will differ depending on your condition and your goals; how you deliver may play a role in your treatment, but not necessarily.
MC: What do you wish more people knew about how physical therapy can help women heal after birth?
CC: Mostly, I just wish people knew that they do not have to experience the postpartum period alone. No one is expected to "figure it out" or "deal with recovery" on their own following an injury or a surgery. Why should birthing a baby be any different? There are physical therapists who understand the human body, what it goes through to make and birth a human, and how to heal and restore function safely and effectively postpartum. I hope we can change the expectation that after delivering a baby you are on your own, because physical therapy is a great resource for all new parents.
MC: What do you advise people recovering from a c-section birth when it comes to recovering at home?
CC: Following a cesarean, some of the most difficult tasks may be everyday activities like getting in and out of bed, coughing, passing bowel movements, or lifting your baby in and out of the crib. When you are recovering at home, it can be helpful to do a virtual session with a physical therapist. Your physical therapist will assess your setup, your equipment, and your needs, and can provide guidance on the best ways to perform those same tasks with less pain, while also protecting your healing body. If you don't have access to a physical therapist, try to listen to your body, use your arms and legs to help perform tasks you would typically rely on your core to perform, and problem-solve any issues early on to prevent forming bad habits or potentially slow healing.
MC: Could you share what your ideal postpartum treatment plan would look like for someone who has just had a c-section birth?
CC: Ideally, I would love to see someone for a virtual session within the first week following cesarean delivery. It can be helpful to speak with a therapist right away to know how to care for the c-section wound, how to promote good healing, and how to perform everyday tasks safely. Additional sessions would be geared towards addressing scar massage and desensitization, rebuilding core and pelvic floor strength, and preparing your body for return to work, sex, and exercise. Working with a therapist once every week or two over the first 8-12 weeks postpartum is a great way to be sure you are setting yourself up for a great full body recovery.
MC: Please can you explain what diastasis recti is. If someone has both diastasis recti and undergone a c-section birth, what would you recommend as a treatment plan?
CC: Diastasis recti is a condition where your rectus abdominus muscles (the 6-pack muscles) are slowly pushed apart, stretching the connective tissue found between those muscle bellies to make space for a growing belly. This happens to almost all people in the third trimester and is not actually a problem in that situation. However, for some people, that tissue between the muscle bellies does not automatically go back to its pre-pregnancy state after delivery: the muscles may remain separated and the connective tissue between them may not be very supportive.
You may continue to have a diastasis postpartum whether you have had a cesarean delivery or a vaginal delivery and, regardless of your birth experience, your treatment plan will be focused on restoring tension to the tissue between the muscle bellies and rebuilding core strength through behavioural modifications and exercise. If you are 8 weeks postpartum and continue to have diastasis recti, meet with a physical therapist to determine a more personalized plan of care to guide you in further closing the gap.
MC: Would you recommend starting physical therapy prior to birth? If someone is having a planned c-section, is there any type of pre-birth protocol that you’d recommend?
CC: I encourage all people to meet with a physical therapist before birth. If for no other reason, learning about your core, your pelvic floor, your diaphragm, and your whole body's function before delivering a baby can be very helpful in making achievable goals and having greater body awareness postpartum. Working with a physical therapist beforehand can also set a great foundation to continue receiving care in the postpartum period, if needed. In the case of a planned cesarean, working with a physical therapist in advance can be especially helpful to learn what to expect and how to care for your body immediately after surgery; trying to learn these strategies in the hospital immediately following delivery, while you are devoting all of your time, energy, and thinking to caring for a new baby, is not always as effective.
MC: Does your therapy approach change if someone is preparing for a c-section birth after c-section (CBAC) or a vaginal birth after c-section (VBAC)?
CC: Having experienced a cesarean delivery does not automatically mean that you will have impairments that would affect future deliveries. If you and your medical provider decide that a VBAC or CBAC is the safest or most appropriate option, then your therapist will support your decision and work with you towards your goals. Your physical therapist is going to assess your body and give tailored guidance and exercises that would best prepare you for your specific birthing plans.
MC: Awareness of the importance of physical therapy seems to be growing– but there’s still a long way to go when it comes to understanding its role in postpartum recovery. Why do you think this is?
CC: First of all, postpartum recovery is not taken seriously in America. There is still a shockingly popular belief that "women have been having children forever and never received help in the past, so why should they need help now?" Of course, you would never hear this same statement in conversations about enlarged prostates or erectile dysfunction. But when it comes to pregnancy, I hear those exact words all the time and from all types of people.
Secondly, good or bad, when someone mentions physical therapy, most people have a general idea of what that is and I can almost guarantee that their first thought is never related to pregnancy or postpartum recovery. It can be difficult to change people's minds about something as simple as seeking help postpartum, or as simple as what it means to work with a physical therapist, and our profession just needs to do better to change both of these public opinions and normalize physical therapy's role in postpartum recovery, but also in every phase of life when dysfunction may occur.
MC: How would you like the landscape of maternal health to look in 5 years from now? What conversations do you want to be happening and how do you see your role in that movement?
CC: When we are unable to participate in our sport or exercise because of an athletic injury or a knee or shoulder surgery, we reach out to a physical therapist in order to help us recover and restore our function. If we are unable to participate in our sport or exercise or have sex or do our jobs or perform basic everyday tasks during pregnancy, postpartum, our menstrual cycle, or menopause, we just deal with it.
I hope that, in the next 5 years, we can at least start to normalize seeking help when women experience pain, incontinence, pelvic pressure or dysfunction at any stage of life. This change is already starting to happen: Women are learning that so many things we have just been expected to deal with in our lives, in our jobs, and in our healthcare, are not at all fair or right, and they are pushing for change. Of course, we still have much further to go, but the conversations have been started; we all just need to do our part to keep pushing forward. As a women's health physical therapist, sharing my knowledge and expertise with anyone and everyone who will listen, like in this interview, is one way I try to help push forward.
Research Articles & Relevant Essays:
My C-Section Was the Happiest Moment of My Life.
Learning the African history of caesarean sections will help us better challenge stigma.
“I was told they didn’t offer C-sections”– the dangerous obsession with ‘natural births. Amid recent maternity scandals, women are speaking out about not being listened to when having a baby– in some cases with terrible consequences
The brilliant Birth Hour podcast shares its collection of women's c-section experiences.
"It's a Battle Scar": The Emotional Toll of C-Sections No-one Talks About.